Among the nightmares of an unprecedented epidemic, sex work gets more dangerous for opioid addicts
Nikki got in the truck after agreeing to exchange sex for $50. She didn’t notice that the passenger-side door handle had been removed until the driver pulled into an empty Home Depot parking lot in Chelsea and pointed a gun at her.
With the gun trained on Nikki’s head, he got out, went around to the passenger side, opened the door, and ordered her to strip to her underwear in the zero-degree weather. He then raped her, drove her back to where they’d met, and dropped her off.
Rather than report the crime to police, Nikki went to her heroin dealer, hoping to get high one last time before starting methadone treatment.
“Some of the stuff we go through out here is just ridiculous,” says Nikki, who asked that her last name not be published. “I don’t know why I’m here. I shouldn’t be. It’s crazy.”
The incident is a stark example of the dangers faced by sex workers—work that both those in the throes as well as outreach and harm-reduction specialists say has grown increasingly chaotic with the rise of the synthetic opioid fentanyl.
Fentanyl’s shorter half life means more injections for drug users. For women like Nikki who do sex work to support their drug addiction, the adjustment has them working more—sometimes constantly—to make enough money to pay for drugs.
Recent studies by researchers in northeastern Massachusetts found an increasing number of women engaging in sex work who report needing to inject more frequently to avoid withdrawal. Angela Bazzi, a professor at the Boston University School of Public Health, says that fentanyl’s shorter half-life can push drug users like Nikki to take more risks to get high.
“Whatever someone was doing to try to make money before fentanyl arrived on the scene, now they just have to do that more often,” Bazzi says. “There’s a greater level of desperation.”
More injections per day means more health risks such as abscesses, infections, and diseases like HIV and Hepatitis C. Adding injury to infection, for sex workers, fentanyl has put an already vulnerable population at more risk for sexual violence.
40 going on 80
Nikki grew up in a typical Italian family in Revere. Her mother and father were high school sweethearts. She spent her weekends working in the garage with her father changing tires and fixing cars, fishing for stripers and bluefish, and riding motocross.
Tall and thin, with wavy dark brown hair and tattooed arms, Nikki has been selling sex to pay for drugs for about 15 years. “It’s not what I wanted to grow up and be,” she says.
Nikki looks younger than her 41 years. But “physically I feel like I’m 81,” she says as she shuffles quickly, hunched over.
It’s not bad posture. Nikki broke her back in a car accident at 21. The steroids she took for her injuries attacked her hip joints and, a couple of years later, she had to have both hips replaced. Doctors told her she wouldn’t be able to have children because of her medical issues, so when she became pregnant with her daughter, Zoey, Nikki called her a miracle baby.
“She was awesome. She was beautiful. She was so independent,” Nikki says.
While her daughter was still young, Nikki and her husband separated, and she began selling drugs to support herself. She also sold to support her own habit. Like many patients, Nikki was prescribed painkillers after her accident and surgeries and wound up addicted.
“We had a house, we had a really nice house. We had money. We didn’t go without, but I was still on drugs,” she recalls.
When she got a settlement from her car accident, she used the money to buy, sell, and use more drugs. Her addiction to OxyContin turned to heroin, and Nikki lost her home and car and eventually had to give up her daughter to her mother.
“This is where my heroin addiction has brought me,” she says.
Before news of the opioid crisis spilled into the mainstream media, to the point that President Donald Trump formed an anti-drug task force last October to pour money into research and treatment, the crisis was relatively hidden. But as is well-known now, behind bathroom cabinet mirrors, in the purses of middle-aged soccer moms, and in the scripts doctors wrote for high school athletes, returning veterans, and injured construction workers lurked an epidemic. Many were just following doctors’ orders and refilling their prescriptions, month after month.
Once marketed as “non-addictive,” drugs like OxyContin were supposed to work miracles, allegedly taking pain away without the addictive side-effects associated with morphine, Vicodin, and other opioids. But investigations into Purdue Pharma, the manufacturer of OxyContin, as well as other companies including major drug distributors, have revealed that these claims were wildly overstated.
Massachusetts is one of more than 40 states suing the company for deceptive marketing and downplaying the risk of addiction. The Sackler family, who founded Purdue Pharma and made billions off the so-called wonder drug, is also being investigated for its role in the opioid crisis. Reports show the Sacklers knowingly kept OxyContin’s addictive strength a secret from doctors and the public.
By the time opioid prescriptions peaked in 2012, doctors had written more than 255 million prescriptions. The National Institute on Drug Abuse reports that about a quarter of people who are prescribed opiates misuse them.
Communities across the country—from big cities in the Rust Belt to small and large communities in the Deep South and on the coasts—have declared public health emergencies because of opioid overdoses and deaths. In 2018, 115 people in the United States died every day from opioid overdoses.
The Northeast has the highest rate of suspected opioid overdoses, concentrated in cities like Chelsea, Revere, and Lynn—three of the poorest communities in Massachusetts, which sit back to back on State Highway 1A north of Boston.
Movies like Manchester by the Sea and Good Will Hunting have romanticized the hardships of New England small-town life, but the reality of concentrated poverty and low-wage work is far bleaker. Whether it’s in a sagging triple-decker or underneath a bridge overlooking the Chelsea River, these cities have become some of the only places in Massachusetts where the underserved and overlooked can find a home.
Deadly and expensive
Outreach workers in Revere say fentanyl started showing up in the area around four years ago and quickly replaced heroin.
Fentanyl, which can be bought online in various forms but is also sometimes acquired through other more local channels, typically originates in China, finding its way to the US through Mexico a lot of the time. Distributors there, not unlike nickel-and-dime dealers stateside, often cut heroin and other drugs with fentanyl. Over the years, cartels in particular have increased fentanyl levels for a stronger, cheaper high. Able to hide perfectly in white powder heroin as well as pills that are fraudulently stamped as medications such as OxyContin, the camouflaged killer makes it impossible for the user to determine whether they are ingesting something fatal. In Massachusetts, a recent study found that more than 90% of opioid overdose deaths involved fentanyl.
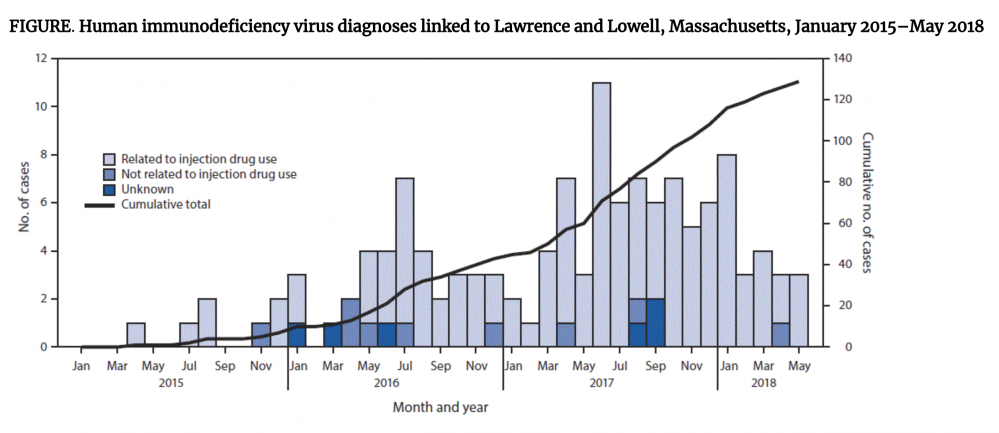
Accidental overdose is only one danger posed by fentanyl. Last August, the CDC announced that an HIV outbreak had been recorded in Lowell and Lawrence, two Massachusetts cities located in what is often considered a major northeastern drug trafficking corridor. Since 2015, the CDC documented 129 new cases of HIV among people in the region who inject drugs. The majority of those infected were 20-39 years old and white, while three-quarters of those interviewed said they injected fentanyl, and 85% of new transmissions of the virus were due to injection drug use.
Researchers found that drug users were injecting up to 10 times a day—a surge that is both deadly and expensive. Chris Alba, an outreach worker with a Lynn-based nonprofit called Healthy Streets, says a bag of heroin, good for one use, currently runs $40 in the Chelsea, Revere, and Lynn area.
Alba, who used to inject, says a heroin high would normally last up to eight hours, so people would mainline about three times a day. The white powder cut with fentanyl that’s on the streets today, however, lasts for only three hours, give or take. Injecting five times a day, at $40 a bag, would cost a user more than $5,000 a month.
So vulnerable, so uncomfortable
On that cold night in January 2018, Nikki was hoping to charge $100 for sex, but settled for $50 because she wanted to get high. The need to use drugs outweighed the risk of getting into a car with a stranger for much less than what she usually charged. Her willingness to work for less isn’t unusual.
“People are now more desperate and experience more trauma to get money,” says Alba.
But when they experience this trauma, many women are hesitant to reach out for help.
Alba says sex workers who are raped often don’t go to the police because they either have active arrest warrants or fear they will be put in jail. As recently as five years ago, state police data showed that in Massachusetts, women are significantly more likely to be charged related to prostitution compared with the men who pay for sex.
And besides, Alba notes, women like Nikki don’t think the police will believe them anyway.
Healthy Streets passes out a “bad date” report based on anonymous reports by sex workers about negative experiences they’ve had with Johns. It’s a long strip of colored paper (the color changes with each updated list) with descriptions of nightmare clients.
“For a lot of women who do street-based sex work, [assault] is part of the job,” says Bazzi. “They might have strategies to avoid it or mitigate but, but it’s common, especially if the woman is suffering from withdrawal.”
“A lot of the women, if they’re really, really sick, sometimes will agree to do certain things they wouldn’t do otherwise, willing to do things without condoms or engage with multiple people, one after the other or at the same time,” says Mary Wheeler, director of Healthy Streets. “Some of the women I talk to say that some men prefer to try to pick them up when they’re sick because they get off on seeing them so vulnerable and so uncomfortable.”
This vulnerability and discomfort is amplified by fentanyl. Many of the women interviewed for this story said fentanyl withdrawal is more intense.
Nic, (not her real name) experienced withdrawal when she went to jail in the spring of 2018. Nic depends on her sex worker partner, N, to support her drug habit.
“I don’t remember the kick being that bad,” Nic, who lives in Lynn, says. “I was puking for days, I couldn’t keep anything down. I don’t remember it being like that. But it was fast. It was like five days. I couldn’t sleep still after that.”
Painful withdrawal from a drug with a shorter half-life leaves women who do sex work to pay for drugs at the mercy of the guy in the next car.
Pink, 28, a former drug user and sex worker, remembers “walking through the blizzards with snow in my Ugg boots, soaked socks, and that didn’t even stop me,” she says. “I just wanted the next one, I wanted the next car. That’s so degrading.”
Pink, whose real name has been withheld, had been sober for five months at the time of our interview. She was taking Suboxone, a prescription drug used to treat opioid dependence, to aid her recovery and working at a restaurant in Cambridge.
Pink’s life has been full of instability. She was sexually abused as a child and started smoking crack at 13. At 15 she tried heroin. Pink managed to kick her opioid habit for a couple of years until she was stabbed eight times in a fight one night in her early 20s. Her pain medication turned into a drug problem, which turned into a heroin problem, which turned into a fentanyl problem.
“It comes hand in hand,” says Pink. “If you have a drug problem, you’re gonna end up hookin’. If you’re hookin’, you’re going to end up getting high. It’s not something that women like to do.”
Sex work is common among women who abuse drugs. A study by the US Department of Health and Human Services found that as many as 80% of women who abuse drugs report a history of sexual and physical abuse.
Pink had moved on from that part of her life by early 2018. She lived in a Revere sober house, an off-white triple-decker with a screen door that slammed every time one of the women residents put on a heavy jacket and walked out to the porch for a smoke break.
But while Pink says her career as a sex worker is behind her, the trauma remains. At the time of our interview, she was working with harm reductionists and trying to find a therapist who could help her with not only her drug addiction, but also with her history of abuse and sex work.
In the summer of 2018, she left the sober house. Danielle Pappas, an outreach worker with Healthy Streets who had helped Pink with her recovery, says Pink is alive. They are still in contact, but Pappas wouldn’t say how she is doing.

Not necessarily safe places
The stigma and shame associated with sex work is a major stumbling block to recovery. When a sex worker goes into a program for fentanyl users, they’re often not equipped to deal with serious trauma. Detox intake and therapy, for example, can cause anxiety for someone who has experienced assault.
“The last thing the woman wants to do is be in a room with no windows and one door with a guy,” Alba says.
The intake process can be brutal, sometimes lasting hours. Patients become nauseous, they start cramping, their bones are hurting, and they’re in a small room with people who ask question after question about their medical history and drug use.
“You’re finally at that stage that you’ve given up and you’re in there, and you’re being interrogated with questions,” Alba says.
On top of that, outreach workers say it’s harder for women to find sober and halfway housing in Massachusetts. After detox, women can choose to participate in an aftercare program, but placement is hard to come by.
As of July, there were 22 halfway houses or recovery homes for women in Massachusetts that were funded by the Department of Public Health’s Bureau of Substance Addiction Services compared to 40 for men. This might seem sensible given overdose statistics—out of 20,571 responses by emergency services for overdoses in the state in 2018, approximately 32 percent of the patients were women—but it doesn’t line up with what Wheeler sees day to day.
“Programs just always say, We can’t keep our female beds full, and I don’t really know if anyone knows why,” she says. “Sometimes it’s easier for women to find places to stay, not necessarily safe places, but places nonetheless.”
Wheeler, who used to strip in downtown Boston and now runs Healthy Streets, got her start in harm reduction by passing out clean syringes and condoms to sex workers in Chinatown.
Harm reduction—a public health approach that accepts illicit drug use is going to happen and focuses on reducing adverse consequences—runs in her family. Her sister, Eliza, oversees the Harm Reduction Coalition in San Francisco and the Bay Area.
These days Wheeler sits behind a desk in the Healthy Streets office, calling cabs for drug users going to rehab, taking smoke breaks outside with her Juul and organizing Narcan training with police departments and nursing students. She is a fierce supporter of the women who walk through the doors of the second-story office in downtown Lynn. Not only does she give them condoms, coffee, and sometimes free clothes, but she also provides unconditional love.
Wheeler says she believes women. All women. “Despite the #MeToo movement and whatnot, women are still kind of told that you are at some level of fault if you were sexually assaulted,” she says. “We’re still kind of given that message … so magnify that by women who are engaging in sex work and substance use.”
Alba, who speaks with a North Shore accent and chain smokes, wears his Healthy Streets identification badge around his neck, along with a small bottle of cologne-smelling hand sanitizer he calls his “manitizer.” He walks the streets of Chelsea, Revere, and Lynn, and carries clean needles, metal containers called “cookers” to dissolve drugs, cotton to strain drugs, and naloxone (also known as Narcan, a nasal spray that counteracts overdoses) in the trunk of his old Jeep. Alba knows most of the people he helps, whom he calls program participants, by their name and an anonymous code used to identify them and track how many people are helped.
Even with the crucial work done by Healthy Streets and other goodwill outfits, the recent HIV outbreak highlighted the need for more harm reduction measures, and pushed the Department of Public Health to increase HIV testing and expand its syringe exchange programs.
Bazzi, who continues to study ways to lift up people who use drugs, thinks more needs to be done. For starters, she is working to make pre-exposure prophylaxis, or PrEP, more readily available for sex workers. If taken correctly, PrEP can help prevent HIV transmission and, by extension, an outbreak.
“We’re not trying to get someone to stop using,” Bazzi says. “We’re just trying to prevent some of the health consequences. We’re trying to keep someone healthy.”
So close
On a summer day in 2018, Nikki discovered that she couldn’t walk, she could only crawl. When she made it to the hospital, doctors told her that an infection caused by injecting drugs made its way to one of her hip replacements. She went septic, and her fever shot up to 104 degrees.
After months in the hospital and four surgeries, the doctors gave up on the infection, which was originally the size of a softball, and decided to take out the entire hip replacement. What’s left is a spacer, not a joint, that is releasing antibiotics to keep the infection from coming back.
Nikki was 102 pounds when she was admitted to the hospital. Two months sober, she was 150, walking with a cane and taking methadone every morning, not only to curb her addiction to drugs but also to provide relief for the pain in her hip.
The hospital stay was a fresh start for Nikki, and for a time she found that her craving for fentanyl had disappeared.
“It’s early in my recovery, and I have no desire to use, but I can’t trust the fact that if I’m around people or places that I won’t want to,” she says.
Nikki found a place to live in a sober house in Revere and stayed away from Chelsea as much as possible. She says she would only let herself hang out with people who had been sober for more than two years and was enjoying the sisterhood the sober house provided. These months were a bright spot.
“I laugh so much more,” Nikki says. “I’m so much more happier. I was so miserable before.”
Not only did she laugh more, she also saw her daughter Zoey, now 16, more. Zoey visited several times a week, and the two began getting to know each other again.“I love her,” she says. “I have no regrets.”
While she was in the hospital, Nikki started knitting blankets to pass time. She says her great grandmother taught her when she was young: “I was just so proud … I know my great grandma is looking down on me and saying, ‘You still got it, kid.’”
But in June, almost a year after Nikki was put in the hospital for the abcess in her hip, she was back on a friend’s couch. Six weeks before, she relapsed.
Nikki says that because she was taking methadone, the doctors wouldn’t prescribe her pain medication. But the methadone would wear off during the day, leaving her in pain. When she asked for more, the clinic denied her request because the script only for heroin recovery, not pain management.
So Nikki went to her former go-to to feel better.
“It just kept spiraling down and down and down, and it’s just really discouraging,” she says.
Nikki’s spacer is long overdue for removal, and she no longer has a date scheduled for her hip replacement. She’s in pain, and says she’s worse off now than a year ago because she can’t do sex work to make a living because of her hip.
All she wants is to get back to where she was this past year, sober and on the way to being pain-free.
“I was starting to get bits and pieces of my life back.”
This reporting was done for the Boston Institute for Nonprofit Journalism and its F.I.G.H.T. Opiates project. For more information, coverage, and videos visit binjonline.org and fightopiates.org.